Sickle Cell Screen Most Popular
The Sickle Cell Screen detects abnormal hemoglobin S in blood to identify sickle cell trait or sickle cell disease. A positive screen suggests the presence of sickle hemoglobin, which may require confirmatory testing. Doctors order this test for newborn screening, genetic counseling, or evaluating anemia, pain crises, or family history of hemoglobin disorders. Results provide key insight into sickle cell status, red blood cell health, and hereditary blood conditions.
- $225.03
- $50.95
- Save: 77.36%
The following is a list of what is included in the item above. Click the test(s) below to view what biomarkers are measured along with an explanation of what the biomarker is measuring.
Also known as: Hemoglobin S
Sickle Cell Screen
The Sickle Cell Screen test contains 1 test with 1 biomarker .
| Please Note: This test is not appropriate for patients less than 6 months old due to interference by Hemoglobin F. In these cases it is suggested that Hemoglobinopathy Evaluation #35489 be ordered. |
Testing Method: Solubility
Collection Method: Blood Draw ![]()
Specimen: 4 mL Whole Blood 
Test Preparation: No preparation required
When is a Sickle Cell Screen test ordered?
Newborns are commonly given sickle cell testing to check for sickle cell anemia. Newborn screening is currently required in all 50 U.S. states as well as the District of Columbia.
When people who were born prior to the requirement for newborn screening wish to know if they have sickle cell disease or are carriers of the sickle cell trait, testing may be done, especially if they are in a high-risk group. According to estimates, one in 500 African Americans has sickle cell disease.
When a person exhibits sickle cell symptoms and/or problems, such as:
- Suffering from sickle cell crises. Painful episodes that might last a long time are among the most typical signs of sickle cell disease. The discomfort can affect any part of the body, although most frequently affects the stomach, lungs, joints, bones, and joints.
- Anemia. Sickle cell disease is a hemolytic anemia, which means that the abnormal, sickled RBCs degrade more rapidly than normal red blood cells and cannot be replaced by the body as quickly as is required. As a result, there are fewer RBCs overall, and their capacity to carry oxygen throughout the body is diminished.
- A rise in the quantity and frequency of infections, particularly pneumonia, the main killer of kids with sickle cell disease.
- Acute chest syndrome, a dangerous consequence of sickle cell disease, is thought to be the source of coughing, chest pain, and fever.
In addition to these symptoms, children's growth issues, leg ulcers in the lower leg, gallstones, and painful prolonged erections of the penis known as priapism may also occur. Because of their distinctive sickle form, sickled RBCs make it difficult for the body to circulate blood through it, which can lead to major consequences. These include splenic sequestration, organ, tissue, or bone damage brought on by a lack of blood flow, as well as stroke, which 10% of children with sickle cell disease experience.
What does a Sickle Cell Screen Blood test check for?
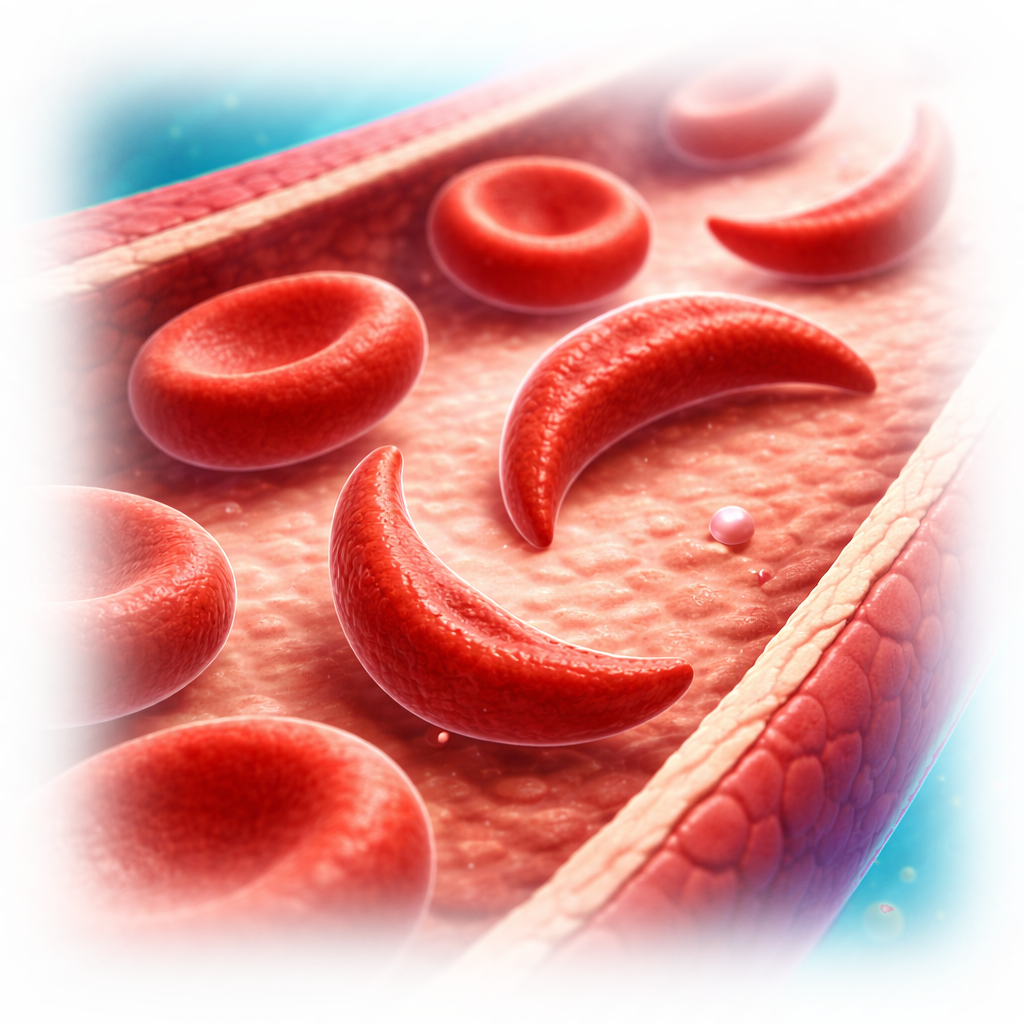 Sickle cell tests are used to identify people who may have sickle cell trait and to aid in the diagnosis of sickle cell anemia. Hemoglobin S is an aberrant hemoglobin that is produced as a result of the genetic disease sickle cell anemia. The existence and relative concentration of hemoglobin S in a blood sample are found out by sickle cell testing.
Sickle cell tests are used to identify people who may have sickle cell trait and to aid in the diagnosis of sickle cell anemia. Hemoglobin S is an aberrant hemoglobin that is produced as a result of the genetic disease sickle cell anemia. The existence and relative concentration of hemoglobin S in a blood sample are found out by sickle cell testing.
Red blood cells include a protein called hemoglobin, which binds to oxygen in the lungs and transports it to other bodily parts. Hemoglobin A typically makes up the majority of the hemoglobin present in adult normal RBCs, with minor levels of hemoglobin A2 and hemoglobin F. Hemoglobin F is often produced in high levels by newborns prior to birth, and Hb A quickly replaces Hb F as the predominate hemoglobin following birth.
Atypical kinds of hemoglobin can result from mutations in the genes responsible for the synthesis of hemoglobin. The mutations that lead to beta thalassemia, a blood condition that reduces hemoglobin production, and mutations connected to hemoglobin variations like Hb S and hemoglobin C are examples of common mutations. A person is considered to have sickle cell trait and to be a sickle cell carrier if they inherit one copy of the normal hemoglobin gene from one parent and one copy of the Hb S gene from the other parent. A person has sickle cell anemia if they have two copies of the Hb S gene. A person will exhibit some of the symptoms of sickle cell disease if they have one Hb S gene and one additional defective gene, such as a Hb C gene.
Sickled red blood cells can be seen in a blood smear.
The RBC can develop crystals of Hb S that take on the distinctive sickle shape instead of its original round disc shape. RBC lifespan is reduced from 120 days to roughly 10-20 days as a result of this altered shape, which also reduces the RBC's ability to travel freely through the body's blood arteries and hemoglobin's capacity to transport oxygen to tissues. Due to the body's inability to create RBCs as quickly as they are being destroyed, a person with sickle cell disease may experience severe anemia. When sickled cells lodge in and block small blood vessels, the affected person may have painful episodes and a number of problems.
To find out if someone is making hemoglobin S and hence carries the sickle gene, sickle cell tests are performed. Every state in the United States and the District of Columbia require them as a standard element of newborn screening programs. One or more sickle cell tests may be prescribed if a newborn screen yields abnormal results in order to confirm the aberrant results. When a person has an unexplained hemolytic anemia or exhibits symptoms that could indicate sickle cell anemia, sickle cell tests may also be requested in addition to or after an abnormal complete blood count and blood smear.
Lab tests often ordered with a Sickle Cell Screen test:
When a Sickle Cell Screen is ordered, it's often part of a broader evaluation of blood health and genetic risk. Here are some tests commonly ordered alongside it:
-
Complete Blood Count (CBC) with Differential:
- Purpose: To evaluate overall blood health, including red and white blood cells, and platelets.
- Why Is It Ordered: To assess for anemia, which is a common symptom of sickle cell disease, and to evaluate the general health of the blood cells.
-
- Purpose: To separate different types of hemoglobin in the blood.
- Why Is It Ordered: To confirm the presence of hemoglobin S (HbS) and to identify other abnormal hemoglobin variants that may coexist, such as hemoglobin C or beta-thalassemia.
-
- Purpose: To measure the number of reticulocytes (immature red blood cells) in the blood.
- Why Is It Ordered: To assess bone marrow function and the body’s response to anemia, which is particularly relevant in sickle cell disease as it causes increased red blood cell destruction.
-
- Purpose: To evaluate iron status.
- Why Is It Ordered: To differentiate between sickle cell anemia and iron deficiency anemia, and to monitor for iron overload, a complication of frequent blood transfusions in sickle cell disease.
-
- Purpose: To measure bilirubin levels, a byproduct of red blood cell breakdown.
- Why Is It Ordered: To assess for hemolysis (destruction of red blood cells), a common feature of sickle cell disease.
-
- Purpose: To measure LDH, an enzyme that can be elevated in tissue breakdown or damage.
- Why Is It Ordered: As an indicator of hemolysis and tissue damage in sickle cell disease.
-
- Purpose: To analyze various components of the urine.
- Why Is It Ordered: To check for proteinuria or other signs of kidney damage, which can be a complication of sickle cell disease.
These tests, when ordered alongside a Sickle Cell Screen, provide a comprehensive evaluation of the condition and its impact on the patient's health. They are crucial for diagnosing sickle cell disease, managing its symptoms, and planning for potential complications. The specific combination of tests will depend on the individual’s symptoms, medical history, and family history.
Conditions where a Sickle Cell Screen test is recommended:
- Sickle Cell Disease: A genetic disorder characterized by the presence of two abnormal hemoglobin S (HbS) genes, leading to the production of abnormal hemoglobin and the associated complications.
- Sickle Cell Trait: Individuals with one normal hemoglobin gene (HbA) and one abnormal hemoglobin S gene (HbS) carry the sickle cell trait. While they usually don't experience symptoms, they can pass the trait to their children.
How does my health care provider use a Sickle Cell Screen test?
A person's red blood cell count, hemoglobin level, and hemoglobin level status can all be assessed using sickle cell testing, as well as whether or not they have one or more mutated copies of the hemoglobin gene. Other aberrant hemoglobin variations might be present, but more testing would be necessary to determine which ones.
Hemoglobin S is one of almost 900 different hemoglobin subtypes. Numerous tests have been developed to detect hemoglobin S and to confirm its presence. Some of these exams include:
Family members of a person with sickle cell trait or disease may be subjected to screening. Additionally, if a person's status is unknown, they may choose to be tested if they were not screened at birth due to the absence of universal newborn screening.
sodium metabisulfite testing and the solubility of hemoglobin S. By introducing specific chemicals to a patient's blood sample that reduce the quantity of oxygen present, both procedures are used to check for hemoglobin S. The aberrant sickle-shaped cells will form as a result of the lower oxygen levels. Individuals who have sickle cell disease will have a lot more hemoglobin S than those who only carry one sickle cell gene. Although this test finds hemoglobin S, it cannot tell if a person has sickle cell disease or a trait. Due to the existence of hemoglobin F, which predominates at birth, it should not be done on newborns until they are at least 6 months old. A premature test may result in a false-negative result because infants with sickle cell disease or trait may not produce significant levels of hemoglobin S until several months after birth.
In order to screen, diagnose, and confirm
Analyses of hemoglobinopathies. The type and relative levels of different normal and pathological hemoglobin types can be determined using a variety of techniques. To identify and measure the many hemoglobin types that are present, these procedures often separate them. They consist of:
The procedure of hemoglobin electrophoresis has historically been used to determine the existence of different hemoglobins.
The most used approach for detecting hemoglobin variations, including Hb S, is hemoglobin fractionation by HPLC.
In big reference laboratories, isoelectric focusing, a highly sensitive technique, is frequently employed.
The District of Columbia and all 50 states in the US currently require newborn sickle cell screening. It determines the various types of hemoglobin present utilizing the more accurate Hb isoelectric focusing or HPLC fractionation. Hemoglobin S levels rise as hemoglobin F levels fall as a baby with sickle cell trait/disease matures and grows. Around age 2, the levels become stable.
DNA examination. This test is used to look at changes and mutations in the genes that create the building blocks of hemoglobin. It can be used to identify whether a person carries one or two copies of the Hb S mutation or two distinct mutations in their hemoglobin genes. The majority of the time, genetic testing is done during pregnancy; to get a clear answer, amniotic fluid may be analyzed between 14 and 16 weeks. If a positive sickle screen from one or both parents is found, genetic counseling is urgently advised. With the use of chorionic villus sampling, it can also be done sooner.
For treatment monitoring
To make sure that the hemoglobin S level has decreased, especially in patients with sickle cell disease, the relative amount of Hb S will be measured and monitored during the course of treatment, such as after a blood transfusion.
Other examinations that could be carried out to assess a person known to have sickle cell disease or trait include:
- Complete blood count. The CBC provides a glimpse of the bloodstream's cell composition. The CBC will assess the size and shape of the RBCs present, as well as how many red blood cells are present and how much hemoglobin is in them. This examination is done to find anemia.
- Iron tests. Iron, ferritin, UIBC, TIBC, and transferrin saturation are examples of these. These tests evaluate many facets of the body's storage and utilization of iron. They are required to assist identify whether a person has iron overload or iron deficient anemia. An iron overload may occur in sickle cell anemia patients who have numerous blood transfusions.
What do my Sickle Cell Screen test results mean?
Infant screening
Fetal hemoglobin F will prevail in neonates who have the sickle cell gene, with a trace quantity of hemoglobin S also present. If they have the sickle cell trait, a trace amount of hemoglobin A can be present. Following the child's sixth month of age, a thorough examination should be performed.
Diagnostic examination
Adults with sickle cell trait primarily generate hemoglobin A that is normal, but individuals with sickle cell illness (anemia) primarily produce Hb S and no Hb A. When a person is heterozygous for two distinct hemoglobin variations, they often produce varied levels of each. For instance, they might make Hb S and Hb C but not Hb A.
Genetic analysis
A person has sickle cell disease if the Hb S gene mutation is found to have two copies. A person has sickle cell trait if they have one gene that codes for Hb S and one normal gene. A person is more likely to have some of the signs and problems of sickle cell disease if they have one Hb S copy and a Hb C or beta thalassemia mutation. A person may or may not experience symptoms or consequences if they have one copy of the Hb S gene plus a different, more uncommon hemoglobin variation. For additional information on this, see the article on hemoglobin abnormalities.
Most Common Questions About the Sickle Cell Screen test:
Clinical Utility and Interpretation
What is the primary purpose of the Sickle Cell Screen test?
The Sickle Cell Screen test primarily detects the presence of hemoglobin S, the abnormal form of hemoglobin associated with sickle cell disease (SCD) and sickle cell trait (SCT).
What conditions or disorders can the Sickle Cell Screen test help diagnose?
The test primarily aids in diagnosing sickle cell disease (SCD) and sickle cell trait (SCT). SCD is a severe hereditary form of anemia, while SCT means an individual carries one abnormal hemoglobin gene but typically does not show severe symptoms.
Clinical Applications and Diagnoses
Why might a doctor recommend a Sickle Cell Screen test?
A doctor might recommend this test if a patient is showing symptoms consistent with SCD or if they have a family history of the condition. It's also routinely done for newborns in many regions as early detection can lead to better management of the disease.
If the Sickle Cell Screen test is positive, what are the next diagnostic steps?
If the screen is positive, further confirmatory tests like hemoglobin electrophoresis or DNA analysis may be performed to distinguish between sickle cell disease and sickle cell trait or to identify other related hemoglobinopathies.
Understanding Limitations and Challenges
What are false negatives and false positives in the context of the Sickle Cell Screen test?
False negatives occur when the test fails to detect hemoglobin S even though it's present. This can happen if a person has a very low amount of hemoglobin S. False positives might occur if the test wrongly indicates the presence of hemoglobin S. Both scenarios, although rare, underscore the importance of confirmatory testing.
How does sickle cell anemia differ from sickle cell trait based on the Sickle Cell Screen test results?
A person with sickle cell anemia will have a majority of hemoglobin S, while someone with sickle cell trait will have both normal hemoglobin (hemoglobin A) and hemoglobin S. The exact proportions can be identified with more specific tests like hemoglobin electrophoresis.
Additional Questions and Insights
Are there populations or groups more prone to sickle cell conditions, and should they be routinely screened using the Sickle Cell Screen test?
Yes, sickle cell conditions are more common among people of African, Mediterranean, Middle Eastern, and Indian descent. In areas or populations with higher prevalence, routine newborn screening and pre-marital or prenatal screening might be recommended to manage and prevent the disease.
How does the Sickle Cell Screen test benefit carriers or people with sickle cell trait?
Knowing one's carrier status (sickle cell trait) is vital, especially for family planning. Couples who are both carriers have a 25% chance with each pregnancy of having a child with sickle cell disease. Awareness allows for informed decisions and early interventions if needed.
We advise having your results reviewed by a licensed medical healthcare professional for proper interpretation of your results.
